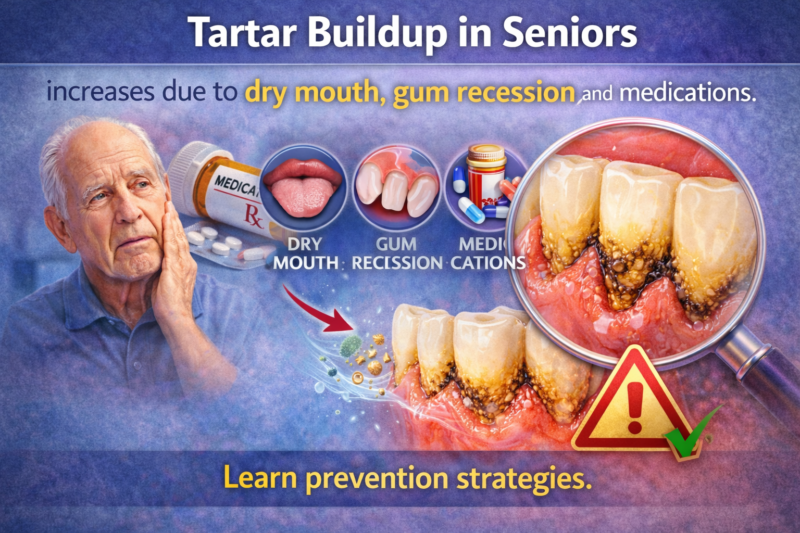
Tartar Buildup in Seniors becomes more common as the body undergoes natural aging changes. Over time, shifts in saliva production, gum health, systemic conditions, and medication use create an environment where plaque hardens more easily into calculus. Because tartar cannot be removed by brushing alone, understanding why tartar buildup in seniors increases is essential for maintaining oral health later in life.
As people age, oral tissues become thinner and more vulnerable. The immune response may also slow, making it harder to fight inflammation caused by plaque bacteria. These factors combine to increase the likelihood of hardened deposits along the gumline.
Gum Recession and Root Exposure
One major reason for tartar buildup in seniors is gum recession. As gums gradually pull back, they expose the root surfaces of teeth. Unlike enamel, root surfaces are softer and more porous.
Exposed roots:
Accumulate plaque more easily
Mineralize plaque faster
Are more prone to sensitivity
Have a higher risk of decay
When tartar forms near exposed roots, it significantly increases the risk of root cavities and periodontal disease. Because root surfaces lack the protective enamel layer, they are more susceptible to bacterial damage once plaque hardens.
Dry Mouth and Medications
Dry mouth is another key contributor to tartar buildup in seniors. Many older adults take medications for blood pressure, heart conditions, diabetes, or anxiety. Several of these medications reduce saliva production.
Saliva plays an important role in:
Washing away food particles
Neutralizing acids
Controlling bacterial growth
Preventing plaque accumulation
When saliva flow decreases, plaque remains on teeth longer. This creates a sticky oral environment where bacteria thrive and mineralization accelerates. As a result, tartar forms more quickly and may accumulate in larger amounts.
Staying hydrated and addressing chronic dry mouth are critical preventive steps.
Limited Dexterity and Oral Hygiene Challenges
Physical limitations can also increase tartar buildup in seniors. Conditions such as arthritis, reduced grip strength, or neurological disorders may make brushing and flossing less effective.
Incomplete plaque removal leads to:
Rapid plaque thickening
Hardened calculus deposits
Increased gum inflammation
Higher periodontal risk
Using adaptive tools can greatly improve daily hygiene. Electric toothbrushes, enlarged handles, and water flossers help compensate for limited hand strength or coordination.
Prevention Strategies for Seniors
Preventing tartar buildup in seniors requires consistent care and regular monitoring. Key strategies include:
Using an electric toothbrush for more efficient plaque removal
Brushing twice daily with fluoride toothpaste
Cleaning between teeth daily with floss or interdental brushes
Staying well hydrated
Scheduling professional cleanings every 4–6 months
More frequent cleanings may be recommended for seniors with periodontal disease or chronic dry mouth. Early maintenance prevents complications and reduces the risk of tooth loss.
 Review the Full Dental Pro 7 Details Here
Review the Full Dental Pro 7 Details Here
If you or a loved one notices increased tartar buildup with age, schedule a professional evaluation promptly. Early intervention protects long-term oral health and helps prevent periodontal complications.
FAQ
1. Why do seniors get more tartar?
Dry mouth, gum recession, and medication use increase plaque retention and tartar formation.
2. Can electric toothbrushes help?
Yes. Electric toothbrushes improve plaque removal efficiency, especially for individuals with limited dexterity.
3. Is tartar more dangerous in older adults?
Yes. Tartar buildup in seniors can accelerate periodontal disease progression and increase the risk of root decay.
